ECIO 2024 will be the venue for a presentation by Dr. Stefano Marcia on the multidisciplinary therapeutic approach to pain in bone metastases, especially in the spine. Several interventional radiology procedures will be demonstrated, including spinal augmentation.
Upstream fromEuropean Congress of Interventional Oncology (ECIO) 2024Which will be held from April 28 to 1any May 2024 in Palma de Mallorca (Spain), keynote speakers present articles related to their favorite specializations.
Various painful restrictions resulting from bone metastases
We have selected Dr. Stefano Marcia, interventional radiologist at SS Trinita Hospital in Cagliari (Italy) on the treatment of bone metastases, a topic he will present at ECIO 2024, on April 28, 2024 at 10:30 am. Bone metastases often lead to severe pain, neurological disability, and loss of mobility, which profoundly affects patients' quality of life. The complex vascular network and venous plexuses of the spine make it particularly vulnerable to metastatic infiltration, which worsens the picture.
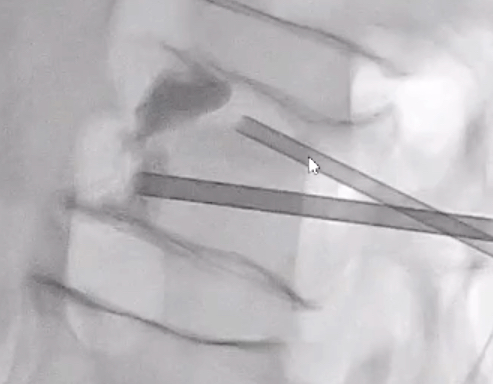 The pathogenesis of metastatic bone pain involves biochemical stimulation of nociceptors, periostitis, and release of tumor-derived cytokines. Therefore, a multidisciplinary approach to the management of bone metastases is essential to achieve optimal patient outcomes. Although conventional external beam radiotherapy remains the primary treatment modality for painful spinal metastases, its effectiveness is variable, with a significant proportion of patients experiencing suboptimal pain relief and recurrence after treatment.
The pathogenesis of metastatic bone pain involves biochemical stimulation of nociceptors, periostitis, and release of tumor-derived cytokines. Therefore, a multidisciplinary approach to the management of bone metastases is essential to achieve optimal patient outcomes. Although conventional external beam radiotherapy remains the primary treatment modality for painful spinal metastases, its effectiveness is variable, with a significant proportion of patients experiencing suboptimal pain relief and recurrence after treatment.
Stereotactic radiotherapy and spinal augmentation complete the multidisciplinary armamentarium
Henceforth, stereotactic radiotherapy (SBRT) is positioned as a promising alternative, despite its association with an increased risk of pathological fractures. When it proves ineffective or contraindicated, percutaneous lumpectomy offers a viable solution, targeting painful lesions, radiation-resistant tumors, and areas highly exposed to radiation. Interventional techniques such as radiofrequency ablation, microwave ablation, cryoablation, or high-intensity focused ultrasound (HIFU) provide acute pain relief while preserving chemotherapy strategies.
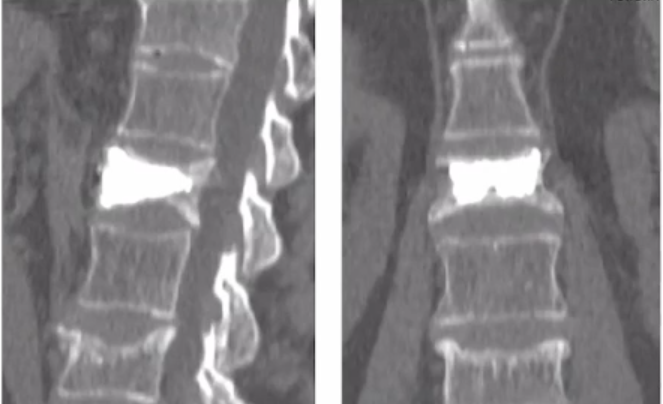
Spinal augmentation – or vertebroplasty – using polymethyl methacrylate (PMMA), is an equally effective approach that stabilizes load-bearing bones and exerts cytotoxic and direct thermal effects on tumor cells and sensory nerves, thus reducing the risk of pathological fractures.
Wallace's algorithm for therapeutic patient selection
 Before any treatment of this type, Dr. Marcia discusses the integration of the Wallace algorithm for therapeutic selection for patients. It provides a structured approach to making treatment decisions, taking into account factors such as life expectancy, performance status, tumor histology, and spinal instability. By integrating this algorithm into clinical practice, healthcare providers can tailor treatments to the individual needs of patients, thus improving treatment outcomes and improving overall satisfaction.
Before any treatment of this type, Dr. Marcia discusses the integration of the Wallace algorithm for therapeutic selection for patients. It provides a structured approach to making treatment decisions, taking into account factors such as life expectancy, performance status, tumor histology, and spinal instability. By integrating this algorithm into clinical practice, healthcare providers can tailor treatments to the individual needs of patients, thus improving treatment outcomes and improving overall satisfaction.
In summary, Dr. Marcia emphasizes that comprehensive strategies for managing bone metastases include a multidisciplinary approach that integrates traditional and emerging treatment modalities. By adopting a structured approach to therapeutic selection and incorporating innovative techniques such as SBRT or percutaneous tumor ablation, health care providers can improve symptom control and improve the overall quality of life of patients with bone metastases.
Bruno Benke

“Subtly charming problem solver. Extreme tv enthusiast. Web scholar. Evil beer expert. Music nerd. Food junkie.”

